Why I filed to run for the US Congress
Grandpa Erick could speak no English, Immigration at Ellis Isl. ask how his name was pronounced – “San’ ness” – so the official stuck out the ‘d’ and told him this was his American name – he was quite happy.
Erick had followed my grandmother who had emigrated the yr. before, she went to N. Dakota and homesteaded a section of land – 640 ac., spent the winter in a sod hut her neighbors helped her build and went to NY to get Erick in the spring.
Erick was the 1st born and would have inherited the very good Sandnes Farm in Snausa – he gave it up to follow his love, Bertine, to the new world.
Bertine was the daughter of Ole the Swede Lap and being 1/4 Laplander she was barred from teaching, govt., medicine, etc. The Laps were Norge’s Negro and her blood was tainted. I’ve a pic. of her on my wall – she was a raving Norge Beauty! She came here alone at 19, 1897, wagon to N.D. and became a wheat farmer, and descendants all over western North America.
I put the ‘d’ back in the name last summer. In 95 I visited the Sandnes farm in Snausa, Norge and learned my grandfather, Erick, had the ‘d’ removed at Ellis Isl. when he came here as an 18 yr. old in 1898. He spoke no English and was very glad to have a new American name.
I have ancestors in the Churchyard in Snausa from the 16th century.
My grandmother, Bertine, came a yr. earlier – she emigrated because, as the daughter of “Ole the Swede Lap”, she was 1/4 Laplander and could not teach, or work in medicine, or govt., etc. – the Laplanders were Norway’s African-Americans.
She got a section of land in N. Dakota, spend the 1st winter in a sod hut some neighbors helped her build, returned to NY in the spring to get Erick. My grandfather was the 1st born and would have inherited the very good family farm in Snausa, he gave up his prince’s inheritance to follow his love.
What a woman! She came here at 19.
Single-payer national health insurance is a system in which a single public or quasi-public agency organizes health financing, but delivery of care remains largely private. Under a single-payer system, all Americans would be covered for all medically necessary services, including: doctor, hospital, preventive, long-term care, mental health, reproductive health care, dental, vision, prescription drug and medical supply costs. Patients would regain free choice of doctor and hospital, and doctors would regain autonomy over patient care.
No. Socialized medicine is a system in which doctors and hospitals work for and draw salaries from the government. Doctors in the Veterans Administration and the Armed Services are paid this way. The health systems in Great Britain and Spain are other examples. But in most European countries, Canada, Australia and Japan they have socialized health insurance, not socialized medicine. The government pays for care that is delivered in the private (mostly not-for-profit) sector. This is similar to how Medicare works in this country. Doctors are in private practice and are paid on a fee-for-service basis from government funds. The government does not own or manage medical practices or hospitals.
The term socialized medicine is often used to conjure up images of government bureaucratic interference in medical care. That does not describe what happens in countries with national health insurance where doctors and patients often have more clinical freedom than in the U.S., where bureaucrats attempt to direct care.
No, single payer will actually save money by slashing wasteful bureaucracy and adopting proven-effective cost controls like fee schedules, global budgets for hospitals, and negotiating drug prices with pharmaceutical companies. The savings – over $500 billion per year on overhead alone – are more than enough to cover all the uninsured. It turns out that it is much more expensive to keep patients away from health care in our current fragmented, market-based system than to provide care to all under an administratively simple single payer system.
Administrative overhead (also known as “transaction costs”) consumes one-third of current health spending in the U.S., a much higher share than in Canada or other nations. A recent paper on hospital administrative costs found that they consume 25 percent of the budgets of U.S. hospitals, compared to 12 percent in Canada and Scotland. Reducing hospital administrative costs to Canadian levels would save $150 billion a year alone.
Over the long-term, controlling the rise in health inflation saves even more money. Without reform, the U.S. is headed towards spending 20 percent of our GDP on health care within a decade (twice as much as other nations with universal coverage), even as we leave 27 million people uninsured and tens of millions more underinsured.
I read “Gold Warriors” by the Sterlings after learning of the Black Eagle Fund and the Hammer Fund in “Black 9/11”. These “black-op funds” started with the gold Japan had amassed from 1894/1945, looted from centuries of Chinese and SE Asia hoarding and buried in the Philippines. Started with $245 billion, dug up by the US military and Ferdinand Marcos, and is now over a trillion.
I think the 9/11 attack was the same kind of thing – the trillions looted from the Pentagon and the gold stolen from the WTC sites. The pattern was there, the banks and drug running in place, and now it’s expanded to several trillions of black op money controlled by this cabal of intelligence agencies allied by their addiction to money and power.
I think it’s an institution of greed and addiction – blaming a family or a caste or a country deflects from the real criminal – us.
The checks and balances to control our ugliness has been gone from America since WWII and perhaps since the rise of the corporation 1880’s. How to recover our form of govt..
The founders knew this would come and tried to design a system, it’s broken down and the result is destroying the planet.
Does it seem odd that the Presidential campaign does not mention:
1) Fukushima – still pouring 100,000 gal. of radioactive water into the Pacific every day – the technology to end the disaster does not exist.
2) How a 47 story building’s fall could be sudden, symmetrical, at free fall acceleration, and completely dismembered in 7 seconds – from office fires?
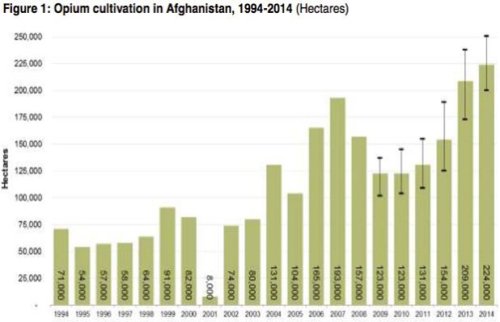
3) The heroin epidemic sweeping America and our presence in Afghanistan where 93% of the planets opium is grown?
I’ve been working for the Sanders campaign since October, buying bumper stickers, making phone calls, talking to Oregonians and FB friends around the world. Tonight Sanders wins in Indiana.
I am certain he will win in Oregon and I think if the Presidential race in the fall is between Sanders and Trump, the Democrats will win the White House in a landslide, both Houses of Congress, and we will be out of the wars within a year.
If the Democrats nominate Clinton, the wars will continue, the Presidential race in the fall will be a toss-up, and the Republicans will retain both Houses of Congress.
Seems like a no-brainer. I wish America’s democratic decisions were based on sense rather than money.
We must reverse “Citizens United”.